Metabolic dysfunction–associated steatohepatitis, or MASH, is an inflammatory, liver-scarring disease that has reached epidemic proportions, with an estimated 1.5% to 6.5% of U.S. adults afflicted by the condition, and roughly 24% of adults having nonalcoholic fatty liver disease (NAFLD).
MASH, previously known as nonalcoholic steatohepatitis, or NASH, is a more serious complication of NAFLD, now called metabolic dysfunction–associated steatotic liver disease, or MASLD. The nomenclature changed recently to reduce the stigma attached to the older terms. Neither disease is associated with alcohol consumption.
What hasn’t changed is the lack of effective treatments. There are no approved pharmacological therapies for MASH, in part due to a lack of adequate preclinical models for study and testing. In a new paper published on December 27, 2023, in The American Journal of Pathology, researchers at Sanford Burnham Prebys, with colleagues at Viscient Biosciences—a San Diego–
based biotech—and UC San Diego and Salk Institute, described a three-dimensional bioprinted liver tissue model employing liver cells from healthy or MASH-diseased donors.
“These tissues display all of the characteristics of MASH, including fibrosis, without any additional disease-inducing agents,” said senior and corresponding study author David A. Brenner, MD, president and CEO of Sanford Burnham Prebys and a longtime leader in liver disease research.
Co-author Jeffrey Miner, PhD, co-founder and chief scientific officer of Viscient Biosciences, underscored the importance of being able to produce a high-fidelity in vitro human primary cell model of MASH. “This approach utilizes the patient’s own diseased cells, allowing them to generate the disease within the bioprinted tissue. We specifically exclude agents that artificially induce disease. We believe this advance enhances the translation of our results to human clinical trials and drug discovery.”
Researchers were able to create their model by layering a mix of primary liver cells and supporting non-parenchymal liver cells (hepatic stellate, liver sinusoidal endothelial and Kupffer) to create bioprinted 3D tissues derived from patient cells.
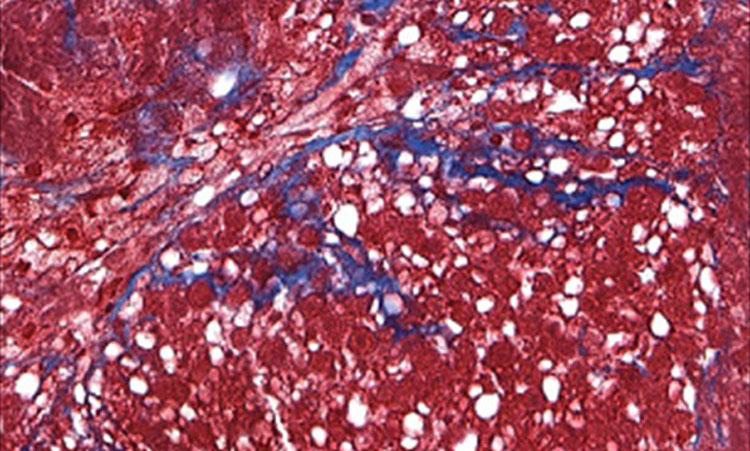
Notably, the resulting diseased tissues displayed fibrosis, an abnormal accumulation of collagen, which in the liver results in progressive scarring and dysfunction, leading to cirrhosis and liver cancer. With no way to stop or reverse fibrosis, the only recourse is an organ transplant.
The new models offered a peek at the underlying pathology, illuminating the roles of hepatic stellate and liver sinusoidal endothelial cells in the disease process.
“This model represents a fully human system with the potential to detect clinically active targets and therapies,” said Miner. “That’s important given that current discovery and animal models have not translated into any approved drugs.”
More about MASLD and MASH
MASLD is a spectrum of diseases characterized by excess fat (steatosis) in the liver. It affects approximately 30% of adults worldwide, with 20% of those patients developing inflammatory MASH that can progress to increasing levels of fibrosis, cirrhosis, liver failure and hepatocellular carcinoma.
In the coming years, MASH is expected to surpass hepatitis C as the main cause of liver transplantation in the United States. The mortality rate of patients with MASH is 7.9%, twice as high as that of the general population. The prevalence of MASH in the United States is estimated to double every 10 years, with approximately 43 million Americans expected to be affected by the disease by 2025.
Additional authors on the study include Philip K. Tan, Traci Ostertag, Haylee Aidnik and Keith Murphy, Viscient Biosciences; Sara B. Rosenthal and Daisy Chilin-Fuentes, UC San Diego; and Sara Linker, the Salk Institute.
The study was supported by funding from Viscient Biosciences, San Diego, California.
Disclosure: Miner and Murphy are co-founders of Viscient Biosciences. Brenner is a scientific advisor. Tan and Aidnik are employees of Viscient; Ostertag is a former employee, and Linker is a former consultant.
The study’s DOI is 10.1016/j.ajpath.2023.12.005.