Hundreds of scientists gather in San Diego and virtually to share knowledge on the science of aging
For scientists in San Diego and across the United States, March 6-7, 2024, is an important time to talk about developments in aging research. To kick off two scientific meetings on the subject, the NIH-funded San Diego Nathan Shock Center, a collaboration among the Salk Institute for Biological Studies, Sanford Burnham Prebys and the University of California San Diego, will host its 2024 symposium focused on the center’s primary research area, “The Heterogeneity of Aging,” on Wednesday, March 6 at the Salk Institute for Biological Studies in the Conrad T. Prebys Auditorium in La Jolla.
Just as people and organisms age at different rates, scientists have demonstrated that tissues also age at their own speeds – even some cells within tissues age at a unique pace. This phenomenon, known as heterogeneity of aging, is of great interest to researchers as it may hold clues for how to develop interventions that enable people to lead healthier lives as they age. to discuss this topic.
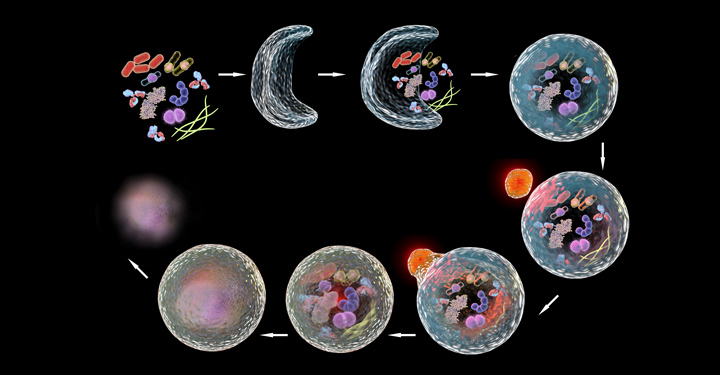
Caroline Kumsta, PhD, assistant professor in the Development, Aging and Regeneration Program at Sanford Burnham Prebys and associate dean of student affairs of the Institute’s Graduate School of Biomedical Sciences, will speak at the 2024 symposium about heterogeneity of aging within the process cells use to recycle or dispose of damaged DNA and other waste products. Kumsta recently coauthored a manuscript in Nature Aging that found new functions for genes involved in this waste management process, known as autophagy. Gaining a better understanding of autophagy is important as scientists have demonstrated that autophagy genes are responsible for prolonged life span in a variety of long-lived organisms. Kumsta received a pilot award from the San Diego Nathan Shock Center in 2022 to support her research on the subject.
“We’re excited to once again offer the La Jolla Aging Meeting on the next day, as we have found that many people like to attend both, and that both meetings help each other,” says Alessandra Sacco, PhD, cohost of both events, director of and professor in the Development, Aging and Regeneration Program at Sanford Burnham Prebys, and dean of the Institute’s Graduate School of Biomedical Sciences.
The 7th annual La Jolla Aging Meeting will be held on Thursday, March 7, also in Salk’s Conrad T. Prebys Auditorium. The meeting was organized by Sacco and Peter Adams, PhD, director of and professor in the Cancer Genome and Epigenetics Program at Sanford Burnham Prebys, and by Jan Karlseder, PhD, Donald and Darlene Shiley Chair, senior vice president and chief science officer at the Salk Institute. The event features mostly short talks from San Diego-based postdoctoral fellows and students researching the biology of aging. The meeting’s goal is to enable participants to meet other researchers and start new collaborations.
“The La Jolla Aging Meeting has more of a focus on early career development, so the events complement each other very well,” adds Sacco.
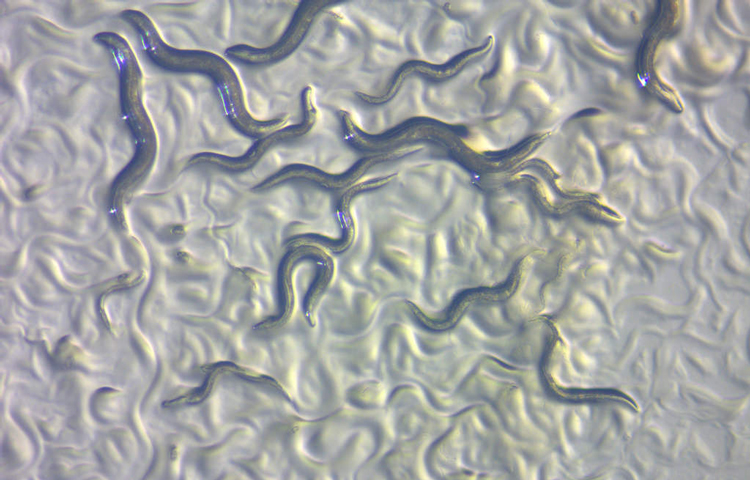
Three members of Sanford Burnham Prebys will be presenting at the La Jolla Aging Meeting, including Xiao Tian, PhD, who recently joined the Institute as an assistant professor in the Degenerative Diseases Program. Tian focuses on epigenomic changes and deterioration that influence age-related diseases by studying the remarkable traits of naked mole rats: They rarely get cancer. They are resistant to some types of pain. They can survive up to 18 minutes without oxygen. And compared to their rodent peers, naked mole rats age very slowly. Tian’s goal is to unravel the molecular basis of aging and develop strategies to promote a healthier, more vital lifespan.
Last year, more than 400 academics, students and trainees at every career stage gathered in person and virtually from 20 states and several countries to participate in the San Diego Nathan Shock Center “The Heterogeneity of Aging” Symposium and the La Jolla Aging Meeting.
About the San Diego Nathan Shock Center
The San Diego Nathan Shock Center (SD-NSC), led by Gerald Shadel, PhD, Audrey Geisel Chair in Biomedical Science and professor in the Molecular and Cell Biology Laboratory at the Salk Institute, was established in the fall of 2020 with the overall goal of understanding the heterogeneity of aging in order to allow development of personalized interventions to increase the number of years of healthy life. To this end, the center provides three novel scientific Research Resource Cores to develop new human cell models of aging and enable the integrated analysis of molecular, cellular and tissue heterogeneity. The SD-NSC also supports and advocates basic biology of aging research in general through the development, training and mentoring activities of a Research Development Core and robust outreach efforts. All of these activities are accomplished via a consortium of three premier research institutions on the La Jolla Research Mesa: the Salk Institute for Biological Studies, Sanford Burnham Prebys and the University of California San Diego.
Alessandra Sacco serves as director of the SD-NSC Research Development Core and Peter Adams serves as codirector of the SD-NSC Heterogeneity of Aging Core.